B.C.’s ambulance service is not meeting targets for patient care, according to a report by the province’s auditor general.
A recent report by Carol Bellringer has pointed out several problems with the service B.C. Emergency Health Services (BCEHS) is offering, including not meeting clinical quality targets.
RELATED: Auditor’s report points to gaps in ambulance service for rural B.C.
The report states that even though BCEHS has developed and tracked clinical quality indicators for several life-threatening conditions, the organization’s performance falls below its targets for most indicators.
“We found that its performance against key targets for patient care needs improvement,” said the report. “Timeliness of response affects patient outcomes, as does the quality of medical interventions provided at the scene and on the way to hospital.”
BCEHS tracks indicators for cardiac arrest, stroke and STEMI — a serious type of heart attack where a major artery is blocked.
Cardiac Arrest
For cardiac arrests, BCEHS tracks performance related to four key indicators.
The organization has set a target for cardiac arrest calls being identified by a call-taker within 60 seconds, 75 per cent of the time. That target is only being met 51 per cent of the time.
The target for a return of spontaneous circulation is set at 50 per cent. BCEHS is meeting that goal with a provincial average of 54 per cent, but missing the mark in certain regions. Return of circulation is only being met 44 per cent of the time in the Interior region and 42 per cent in the Northern region.
A 75-per-cent target has been set for paramedic response times for cardiac arrest calls falling inside of established response time targets. Response time targets are nine minutes for urban, 15 minutes for rural and 30 minutes for remote.
Response time targets are met 57 per cent of the time in the Fraser health region, 72 per cent of the time in the Interior region, 79 per cent in the Vancouver Island region, 74 per cent of the time in the Northern region and 75 per cent of the time in the Vancouver Coastal region.
The final target is for CPR to be performed by bystanders, but BCEHS indicated there was no clear trend to report for that indicator.
Stroke
Four indicators for strokes are also measured.
A target for the recording of blood sugar checks is set at 100 per cent. The provincial average is 86 per cent, with most health regions falling just slightly above or below that number.
The target for documenting the onset of symptoms is also 100 per cent. Province wide, that target is only being met 55 per cent of the time. The Northern region had the lowest number at 38 per cent, with the rest of the regions close to the provincial average.
A 100-per-cent target is also set for giving oxygen according to stroke protocols. That is being met 52 per cent of the time in the Northern region, 69 per cent of the time in the Fraser region, 70 per cent of the time in both the Interior and Vancouver Coastal regions and 72 per cent of the time in the Vancouver Island region.
The final stroke target is for on-scene time to come in at less than 20 minutes. Province-wide that timeline is met 69 per cent of the time, however the goal is 80 per cent.
STEMI
The final indicators included in the auditor’s report are for STEMI.
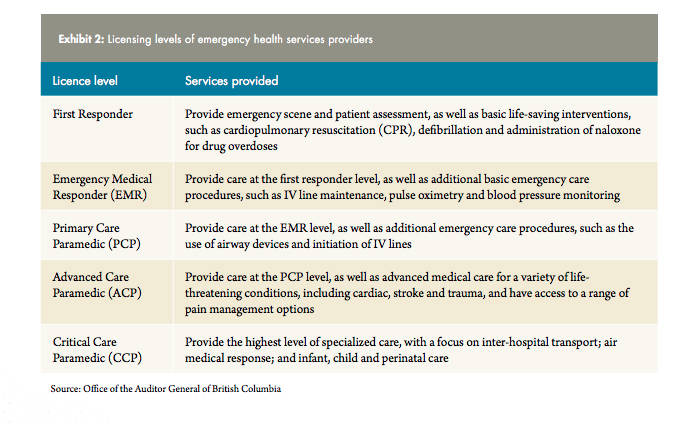
In this province, only advanced care and critical care paramedics are licensed to perform STEMI recognition.
Because advanced care paramedics are not stationed in rural and remote communities, STEMI recognition and treatments are not even available for a large portion of the province, so these indicators only reflect the areas with advanced care paramedics.
The auditor’s report acknowledges the lack of advanced paramedic staffing in rural communities may put some patients at greater risk.
“Timely diagnosis and transport to an appropriate hospital improves the likelihood of patient survival,” emphasizes the report.
It also says BCEHS has not evaluated its advanced care coverage to determine whether it is sufficient to meet the needs of patients requiring higher-level care across the province.
RELATED: Policy prevents advanced paramedic care in rural areas
BCEHS is almost making its 90-minute target for the time from the arrival of an advanced care paramedic to the delivery of the patient to an appropriate hospital.
The target for an advanced care correctly diagnosing STEMI is 80 per cent, with provincial numbers coming in at 72 per cent.
The organization is reaching its goal for false-negative diagnosis being correctly overridden by an advanced care paramedic 40 per cent of the time.
Changes since audit
After the audit was done, but before the report was issued, BCEHS introduced several new initiatives.
According to BCEHS, this includes 119 regular paramedic positions, more than 100 specialized paramedic positions including community paramedics, 20 emergency dispatchers and six nurses to triage less urgent calls.
The additional 119 paramedics, which are made up of both part-time and full-time positions, is an increase of about three per cent to the number of paramedic positions in the province.
By BCEHS’s own calculations, the organization expects call demand to increase by over six per cent annually.
In the first half of 2018 BCEHS also introduced a new dispatch prioritization process and automated the recording of arrival times at the scene in order to more accurately capture response times and increase confidence in data collected.
The auditor reviewed response times to see if they had improved with these initiatives and found only a slight improvement in response times during 2018 with 51 per cent of responses to high-acuity events in urban areas coming in under nine minutes, compared with 50 per cent for the audit period.
“During the audit period, BCEHS was in the early stages of launching the plan and seeing positive results,” said BCEHS executive vice president Linda Lupini in a response to the report. “We expect these improvements to continue as we move into the next phases.”
She also stated the organization is committed to following up on the report’s recommendations to make services even better.
betsy.kline@castlegarnews.com
Like us on Facebook and follow us on Twitter