Editors note: This article has been updated with comments from the Ministry of Health.
A group of doctors and health experts that don’t agree with the province’s handling of the pandemic are calling for better use of the expiring supply of B.C.’s rapid antigen tests, in addition to the current vaccine mandates.
In their third news conference on Wednesday (Nov. 3), Protect our Province B.C. said that only 10 per cent of the 3,147,706 rapid antigen tests B.C. received from the federal government have been used so far in the pandemic.
The province disputes those numbers, saying B.C. has received 2,796,506 rapid tests from Health Canada and a total of 1,301,089 tests have been deployed and as of October 30, 2021, approximately 429,795 rapid tests had been used with 1,781 presumptive positive results.
Dr. Victor Leung, an infectious disease physician and medical microbiologist, explained that COVID often reaches its highest level of infectiousness before the onset of symptoms. In B.C., people are often only given PCR tests for COVID once they become symptomatic, meaning that much of the transmission had already occurred before their cases were detected.
RELATED: Health experts launch B.C. COVID briefings out of ‘growing concern’ with government response
RELATED: B.C. defends COVID rapid testing program as more than a million kits sit in storage
Public health measures like B.C.’s vaccine card and vaccination mandates for staff in long-term care and healthcare settings have been put into place to curb the spread of COVID.
However, the COVID-19 vaccine isn’t 100 per cent effective, meaning no one is entirely covered from contracting or transmitting the virus even when fully vaccinated. PoP B.C. recommends using rapid tests as another layer of protection on top of vaccination.
Meanwhile, Health Canada guidelines dictate that rapid tests must carry a minimum 80 per cent accuracy.
Paul Tupper, a SFU mathematics professor and member of the BC COVID-19 Modelling Group, said modelling shows rapid antigen tests have the potential to reduce COVID cases being transmitted by staff in long-term care by 50 per cent.
Rapid antigen tests could be utilized as an additional protection measure for sporting events, weddings and in schools, as well as spaces where vulnerable people gather such as shelters and senior’s homes.
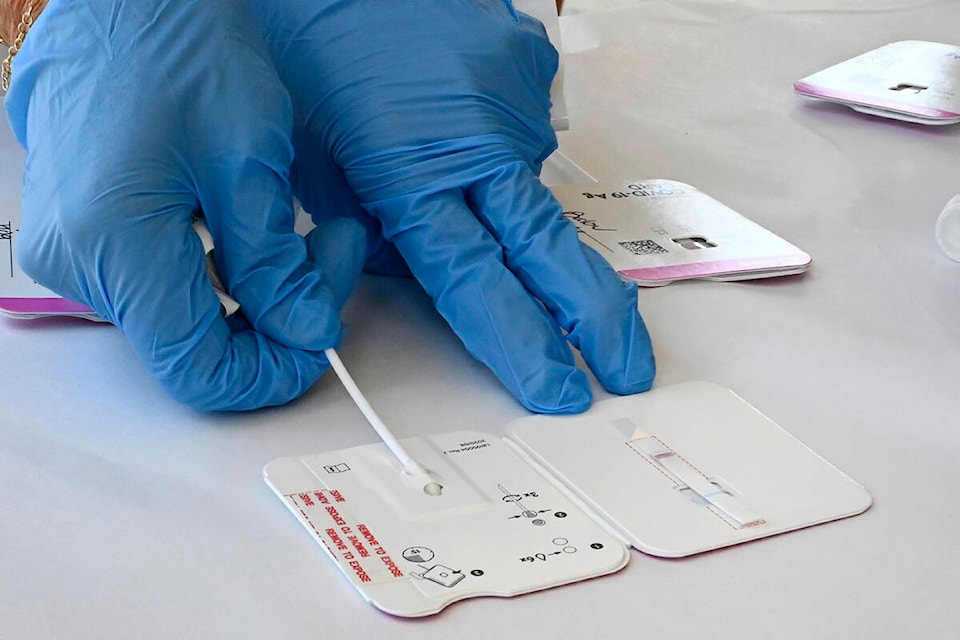
If the tests, which take about 15 minutes to produce a result, were made available prior to entry and someone were to test positive, it would prevent a possible transmission while that person isolates and gets confirmation through a PCR test.
Dr. Lisa Barrett, an infectious disease specialist with Dalhousie University, told reporters that rapid tests in Nova Scotia have been successful throughout the pandemic, including building trust and access when the vaccinations were rolled out.
RELATED: B.C. waiting for new rapid tests to be approved before large-scale rollout in schools
RELATED: Why Atlantic Canada excels at slowing the spread of COVID-19
She urged all jurisdictions to make use of rapid tests if they have them available.
“Just do it. Don’t worry about having a perfect distribution system. Don’t worry about the test sensitivity. It’s 100 per cent better than doing no tests in people who have no symptoms. Let people lead in the community and I think you’ll see the dividends go beyond just diagnosis and testing to actual trust, involvement and engagement.”
PoP B.C. called on the public to write their MLAs, their local medical officers of health and the public health office asking the province to deploy rapid antigen tests more widely in B.C.
The controversial group has faced criticism for holding alternate briefings that criticize the government’s COVID-19 response. Critics are concerned that the briefings could undermine public trust in the government at a time when building trust is key.
Dr. Amy Tan is a palliative care & family physician, clinical associate professor with the UBC faculty of medicine and a member of the PoP B.C. steering committee. Tan said the group’s goal is to share the best available science on COVID-19, not undermine the government.
“We’re just asking for transparency. We’re asking how these decisions are being made. From our vantage point as health professionals and scientists, we’re seeing the science is different.”
A spokesperson for the ministry of health said they are “aware” of Protect our Province and that they welcome scientific evidence to protect people against COVID-19. They said B.C. has been following guidelines from the World Health Organization, Health Canada, the Public Health Agency of Canada and the National Advisory Committee on Immunization among others.
The spokesperson said B.C. is “fortunate” to have a public health team led by provincial health officer Dr. Bonnie Henry, adding that Henry takes all evidence presented to her seriously.
“We will continue to listen to public health experts like Dr. Henry, the many teams she works with, and the local, national, regional, and global bodies that provide information, guidance, and expertise. As we have always done, we advise people to seek out information from credible, well-informed public health experts and sources.”
The ministry confirmed they have not met with PoP B.C. and made no commitment to do so.
When asked if PoP B.C. would be willing to meet with the government despite several invitations from the group already going unanswered, Tan replied: “Absoutely.”
RELATED: B.C. reports 406 new COVID cases, 5 deaths as first doses reach 90%
@SchislerCole
cole.schisler@bpdigital.ca
Like us on Facebook and follow us on Twitter.
Want to support local journalism? Make a donation here.